Pityrosporum Folliculitis
What is Pityrosporum Folliculitis?
Pityrosporum Folliculitis is currently known as malassezia folliculitis. Pityrosporum Folliculitis is a skin condition characterized by itching and acne like flare-ups in hair follicles. Malassezia folliculitis appears as tiny pink papules and pustules on your chest, back and shoulders. It can also affect other areas such as your upper arm, face and neck1, 2, 5.
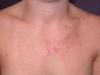
Pityrosporum folliculitis is caused by a yeast species known as Malassezia furfur. These species thrive in sebaceous environment since they convert triglycerides into free fatty acids and feed on them as a result cause inflammation in those areas.
Malassezia is found on the skin of health people. They are present on the skin immediately after birth and become many in late adolescence and early in adulthood.
Particular climate plays a key role in influencing the number of people with Pityrosporum folliculitis. People living in humid and warm environment are largely affected by pityrosporum folliculitis.
Pityrosporum folliculitis affects young and middle-aged adults and youths. This condition is common in people who are 15-45 years of age. Both male and female are affected.
Causes
Malassezia folliculitis causes are not yet understood. However there are factors that are believed to promote growth of yeast on the skin of people. They include the following:1, 2, 5
Internal factors
Medications
Use of certain medications can promote pityrosporum folliculitis. Drugs such as oral antibiotics are used to kill skin bacteria but not yeast. This allows yeast to reproduce and attack your skin causing pityrosporum folliculitis. For example long term use of tetracyclines can encourage the growth of malassezia.
Another medication is oral contraceptive which is a birth control drug that is used to prevent pregnancy. These medications has estrogen and progestin component. Although oral contraceptives are used in preventing pregnancy, they can also treat skin disorders. However oral contraceptives can cause other skin conditions including pityrosporum folliculitis.
Oral steroid used to treat severe acne can also promote reproduction of yeast on your body and cause pityrosporum folliculitis.
Obesity
People who are overweight tend to sweat more. The sweat provides a favorable environment for this yeast to thrive and reproduce.
Immunodeficiency
This is where the ability of your body to defend against infection is greatly reduced and therefore makes you more prone to bacterial, viral and fungal infections. Immunodeficiency conditions are either acquired or inherited. Acquired immunodeficiency you obtain them as you live while inherited immunodeficiency is that which is passed to you at birth.
Therefore those people with a weak immune system are at greater risk of developing pityrosporum folliculitis.
Systemic candidiasis
This refers to a group of yeast infections that affect your brain, heart and any other part of your body. It is mostly caused by Candida yeast. This yeast lives on the skin and in your digestive system and usually do not cause any problem. When Candida yeast finds its way into your blood, it reproduces and spreads to other parts of your body. As a result it can cause pityrosporum folliculitis.
Diabetes mellitus
This is a condition that lowers the ability of your body to utilize energy in food. Diabetes mellitus are grouped into the following: gestational diabetes, type 2 diabetes and type 1 diabetes.
All these kinds of diabetes have a common thing. Usually, your body metabolizes carbohydrates and sugars you eat into glucose. Glucose provides energy to the cells in your body. The cells need insulin, a hormone that enables the cells to absorb glucose and use it for energy. However, with diabetes mellitus, your body is either not able to make adequate insulin or use it.
Since your body cells cannot absorb glucose, it accumulates in your blood. These increased levels of glucose in your blood can damage your blood vessels in your heart, kidney, eyes and nervous system.
External factors
- Humid and warm climate: People living in humid and warm environments sweat more. This sweat provides a conducive environment for yeast to flourish and reproduce.
- Tight clothing: People who wear very tight clothes sweat more and are more vulnerable to pityrosporum folliculitis.
Other external factors that can promote pityrosporum folliculitis include:
- Applying coconut oil and greasy sunscreens on the skin provides oil that this yeast feeds on and reproduces.
- People with an oil skin are more likely to develop pityrosporum folliculitis since the yeast like feeding on skin oil.
Diagnosis
Pityrosporum folliculitis can be diagnosed through a physical exam and other tests. In physical exam, your doctor examines your skin for the symptoms that are associated with pityrosporum folliculitis.
Your doctor can also do a skin biopsy to find out the type of infection present and rule out other similar skin conditions. In skin biopsy, your doctor scratches a sample of the affected skin on either your chest, neck or upper arm and take them for pathological analysis. For accurate results, your doctor can remove a pustule from the affected area and examine its content under a microscope
Treatment
Pityrosporum folliculitis can be managed effectively when treatment is focused on treating the underlying factors that promote the growth of yeast on the skin and prevent its recurrence. The following can be used to treat pityrosporum folliculitis:
Antifungal drugs
There are many types of antifungal drugs that you can choose from to help cure pityrosporum folliculitis. They include:
Ketoconazole
It is effective in stopping every species of Malassezia. To use this drug, apply only 2% of ketoconazole shampoo two times a week and continue for four weeks on the affected area. When the lesion on your skin has disappeared, continue using ketoconazole for once a week for better results. In addition, leave the solution on your skin for about five minutes and then rinse it off.
Other antifungal medications you can use include:
- Climbazole
- Butenafine Hydrochloride
Natural Treatment
There are a number of natural products you can use to mange Pityrosporum folliculitis at the comfort of your home. They include:
Tea tree oil
Tea tree oil has antimicrobial properties to fight against Malassezia furfur. To use tea tree oil, dilute it first and make sure it is about 1% concentration and apply on the affected area.
Honey
To use honey, put raw honey with water on the affected area for three hours daily and continue this for four weeks. This will cure the lesions on your skin. Since there is high chances of relapse, make sure you continue using honey once each week for seven months. Alternatively, you can try other products that have honey extracts.
Pictures



Reference List
- Pityrosporum Folliculitis. Available at https://simpleskincarescience.com/pityrosporum-folliculitis-treatment-malassezia-cure/
- http://www.aocd.org/?page=PityrosporumFollicu
- https://www.dermnetnz.org/topics/malassezia-folliculitis/
- Pityrosporum Folliculitis Treatment. Available at http://emedicine.medscape.com/article/1091037-treatment
- Pityrosporum Folliculitis. Available at http://emedicine.medscape.com/article/1091037-overview#a2
