Iridocyclitis
What is Iridocyclitis?
Iridocyclitis along with iritis (inflammation of the iris alone), can be less specifically called anterior uveitis as it affects the front part of the eye and is the most common type of uveitis, predominantly occurring in young and middle-aged people. Many cases occur in healthy people and may only affect one eye but some are associated with rheumatologic, skin, gastrointestinal, lung and infectious diseases. [7,8,9]
First, take a look at the two main parts affected by iridocyclitis:
The iris (plural: irides or irises) is a thin, circular structure in the eye that is responsible for controlling the diameter and the size of the pupil which means it is responsible for controlling the amount of light reaching the retina.
In optical terms, the pupil is the eye’s aperture (an opening that controls the amount of light that passes through a lens), while the iris is the diaphragm (controller of the amount of light passing through the lens that serves as the aperture stop. [1, 2]
Nice to know: Eye color is defined by that of the iris [2]

Figure 1 Eye Structures – Front view and lateral view of the eye
The ciliary body is a part of the eye that includes the 1.) ciliary muscle, which controls the shape of the lens (the clear part of the eye that focuses light to form clear images, and the 2.) ciliary epithelium which produces the aqueous humor (thin, watery fluid produced in the eye).
The ciliary body is also a part of the uvea, the layer of tissue that delivers oxygen and nutrients to the eye tissues. The ciliary body is connected to the ora serrata of the choroid and to the roots of the iris. [3,4,5]
Iridocyclitis causes disturbance of the funtions of iris such as “photophobia” and the ciliary body such as “blurred vision”. There are two types of iridocyclitis : nongranulomatous and granulomatous.
The most common type of iridocyclitis is the nongranulomatous type, which manifests as an acute condition with pain, photophobia and a pattern of conjunctival injection, especially around the cornea. The pupil is small, fine precipitates on the posterior corneal surface and cells in the aqueous humor.
If severe,a hypopyon (ie, accumulation of pus in the anterior chamber) may occur. The condition may be unilateral or bilateral and may be recurrent. Repeated attacks can cause anterior synechia (ie, peripheral iris adheres to the cornea and impedes outflow of aqueous humor).
On the other hand, granulomatous iridocyclitis tends to be chronic and has a more insidious onset. Symptoms such as photophobia and pain may be minimal. The keratic precipitate may be larger and grayish in color. Vision is markedly and adversely affected. [16]
What is Fuch’s Heterochromic Iridocyclitis?
Fuch’s Heterochromic Iridocyclitis is characterized by idiopathic non-granulomatous anterior uveitis. It has an insidious onset and occurs recurrently. Most of the cases occur in young females. It is mostly mild and unilateral, and people affected commonly complain blurred vision.
Classical presentation of uveitis in Fuchs heterochromic iridocyclitis is infrequent to 1+ anterior chamber cells, aqueous flare of 1+ to 2+, diffuse white stellate keratic precipitates on the endothelium which are non-pigmented non-confluent in nature.
The pathognomic sign of Fuch’s Heterochromic Iridocyclitis is the absence of posterior. Most patients present with posterior subcapsular cataract in early stages and with total white cataract in advanced stages. Intraocular pressure (IOP) is usual in early stages but in late stages there is increase in IOP which is usually refractory to medical and even to surgical therapy.
There can be vitreous haze with Fuchs heterochromic iridocyclitis. Most cases with Fuchs heterochromic iridocyclitis do not require any topical steroids to control inflammation as iridocyclitis is manageably mild and most commonly aqueous flare.
Vitreous haze also does not require any systemic steroid treatment. Outcome of cataract surgery in Fuchs heterochromic iridocyclitis is usually positive. The hallmark of the disease due to iris stromal atrophy is Heterochromia iridium. [17,18]

Causes
Several factors can be cited as the possible cause/causes of iridocyclitis. Basically those factors trigger the inflammatory response of the body which causes the iris and the ciliary body to be inflamed. These include:
- Immune system problems- Iridocyclitis may happen with people who have underlying autoimmune condition. Autoimmune response is triggered when the body mistakenly attacks its own healthy tissues, and it usually has no known cause.
- Examples of autoimmune diseases that lead to iridocyclitis include: Ankylosing Spondylitis, Reactive Arthritis, Psoriasis, Multiple Sclerosis, Behcet’s Disease, Sarcoidosis, Juvenile Idiopathic Arthritis
- Infections- Iridocyclitis can be caused by germs (bacteria, viruses, parasites, etc.) that enter the body affecting thee iris and the ciliary body. Herpes zoster or herpetic Iridocyclitis is one such infection which might affect the pupil and cause distortion. This can also happen alongside systemic infections such as toxoplasmosis, tuberculosis, and rarely, HIV and syphilis.
- Trauma or injury to the eyes, or eye surgery
- Drug related side effects such as:
- Rifabutin, a derivative of Rifampin
- Use of quinolones especially Moxifloxacin according to several reports
- All of the widely administered vaccines have been reported to cause iridocyclitis.
- Some types of cancers, such as lymphoma, although this is a very rare cause of iridocyclitis.
- Sometimes, a specific cause of iridocyclitis cannot be identified. [10,11]
Signs & Symptoms
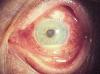
Figure 2 – Person’s eye with iridocyclitis
Signs:
- Redness of the eye
- Lacrimation
- Constriction of pupil
- Dilated ciliary vessels in which the anterior chamber contains cells and flare, as well asold episode keratic precipitates (“KP”) on the posterior surface of the cornea. In severe inflammation there may be evidence of a hypopyon. Previous episodes of iridocyclitis are identified by pigment deposits on lens, KPs, and festooned pupil on dilation of pupil.

Figure 3 – Keratic precipitates of an eye with iridocyclitis
- Busacca nodules, inflammatory nodules located on the surface of the iris in granulomatous forms of anterior uveitis such as Fuchs heterochromic iridocyclitis (FHI).[4]
- Synechiae- eye condition where the iris sticks to either the cornea or lens

Figure 4 – Right eye of patient with uveitis showing localized area of posterior synechiae
Symptoms:
- Burning sensation in the eye affected
- Blurry vision
- Photophobia
- Irregular pupil
- Blacked out sclera
- Floaters, which are dark spots that float in the visual field
- Headaches [12,13,14,15]
Diagnosis
- Dilated Fundus Examination may be done to rule out posterior uveitis. Results present white spots across the retina along with retinitis and vasculitis.
- Discovering any underlying causes. This evaluation physical examination, complete systems review, and diagnostic tests including a complete blood cell count, erythrocyte sedimentation rate, antinuclear antibodies (ANA), VDRL, and Lyme disease titer.
- Underlying causes include toxoplasmosis, herpes zoster virus, ocular candidiasis, histoplasmosis, herpes simplez virus, tuberculosis, and syphilis. [19, 16]
Treatment
Iridocyclitis is usually treated with a topical eye drop containing glucocorticoid steroid such as prednisolone acetate. This can also be in oral form. Local corticosteroid drops, such as Pred Forte 1% and Flarex 0.1%, instilled four to six times a day are used to decrease inflammation. In very severe cases, systemic corticosteroid or intravitreal corticosteroid may be used.
Patients are advised to wear dark glasses outdoors to prevent photophobia. Synechia and ciliary spasm can be avoided with the use of midriasis such as cyclopentolate(Cyclogyl) and atropine. [19,16]
Complications
If left untreated, Iridocyclitis may lead to:
- Glaucoma
- Cataract
- Brand Ketaropathy- corneal disease derived from the appearance of calcium on the central cornea
- Macular Edema- occurs when fluid and protein deposits collect on or under the macula of the eye and causes it to thicken and swell (edema)
- Permanent Vision loss [16,19,20,21]
References:
- 2017, Meriam-Webster, Inc.
- eye, human, “Encyclopedia Britannica” from Encyclopedia Britannica 2006 Ultimate Reference Suite DVD
- Cassin, B. and Solomon, S. Dictionary of Eye Terminology. Gainesville, Florida: Triad Publishing
- http://www.healthline.com/human-body-maps/eye-vitreous-and-aqueous-humor
- http://www.brightfocus.org/glaucoma/infographic/flow-aqueous-humor
- http://www.rightdiagnosis.com/i/iridocyclitis/basics.htm
- http://www.webmd.com/eye-health/uveitis-inflammation-eye#1\
- Leffler CT, Schwartz SG, , Davenport B, Spetzler K, Stackhouse R. (2013). “Evolution and impact of eye and vision terms. JAMA Ophthalmol. 131 (12): 1625–31. doi:10.1001/jamaophthalmol.2013.917. PMID 24337558
- https://www.hxbenefit.com/iridocyclitis.html
- http://www.nhs.uk/Conditions/Uveitis/Pages/Causes.aspx
- Abdullah Al-Fawaz and Ralph D Levinson. “Uveitis, Anterior, Granulomatous”. WebMD. (15 December 2010)
- https://en.wikipedia.org/wiki/Synechia_(eye)
- http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v9/v9c004.html
- http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v9/v9c003.html
- Suzanne C. Smeltzer & Brenda G. Bare: Brunner & Suddarth’s Textbook of Medical-Surgical Nursing,10th Edition Volume 2
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2841369/
- Hogan M.J., Kimura, S.J., Thygeson P. Arch Ophthalmol. 1955;53:179–86. [PubMed]
- https://en.wikipedia.org/wiki/Uveitis#Diagnosis
- Digital Reference of Ophthalmology
- What Causes Macular Edema”. American Academy of Ophthalmology. 30 January 2016
